Welcome to the Canadian Hair Transplant Centre
With over 3,800 hair restoration surgical procedures to his name, and an extensive background in family and emergency medicine, he believes that a hair transplantation when performed by an experienced doctor with precision and artistry, can do wonders for a person’s appearance, well being and self esteem.
Dr. Simmons is passionate about making sure that every hair transplant he performs leads to outstanding, undetectable results for his patients. To learn more about how we can help you with your hair loss challenges please feel free to contact us or call anytime for a free and discreet consultation.
HAIR TRANSPLANTS
Facts & Alternatives
The psychological importance of hair is significant in many cultures worldwide. Most of us have a personal or emotional connection to our hair and we appreciate that it can positively and negatively influence our appearance and quality of life.
Learn more about hair loss facts and alternative options to surgical solutions...
 Consequences
Consequences
of Hair Loss
 What is Androgenic Alopecia?
What is Androgenic Alopecia?
 Facts About Finastride Propecia
Facts About Finastride Propecia
 About Minoxidil (Rogaine)
About Minoxidil (Rogaine)
 Facts About Laser Therapy (LLLT)
Facts About Laser Therapy (LLLT)
 Platelet-rich Plasma (PRP)
Platelet-rich Plasma (PRP)
 Surgical Treatment of Baldness
Surgical Treatment of Baldness
 Hair Transplant Self Evaluation
Hair Transplant Self Evaluation
 Medical
Medical
References


Stephanie Gogo
01:46 24 Sep 19
I had a hair transplant by Dr. Simmons about 10 years ago. ... It was much more painful than he described to me especially in the back of my head where the donor hair was taken from. For the first couple of years my hairline looked great however my scalp was extremely tight and I had headaches. After a couple of years my scalp began to loosen and the headaches went away however my hairline changed as well. It looks the same as before the transplant or even worse in my opinion. I contacted his office numerous times after seeing the changes in my hairline. His receptionist never put me through to him and he never answered any of my emails. My photo is still used as a before and after. My hairline no longer looks like the after photo.read more
imran aslam
21:21 03 Mar 19
I am a very satisfied customer of CHTC. The doctor and his... team of professionals are very disciplined and provide a comfortable and caring environment for your H.T. procedure. I would recommend CHTC to anyone who is interested in dealing with their hair loss and thinking of an H.T. procedure.read more
Sukhjinder Kande
15:30 17 Feb 19
I had a hair transplant at this clinic. The doctor and... staff were very professional. I had a great experience. I would highly recommend this clinic to anyone looking to having a hair transplant. STransread more
Peter Crowe
09:24 03 Feb 17
I am quite Happy with the results of my FUT hair transplant... in Oct of 2015, I would recommend the Canadian Hair Transplant Centre to anyone, I got a great deal for a very good result, thank you to everyone at The Canadian Hair Transplant Centre, especially Dr. Simmons.read more
MALE | Norwood 3 - MALE VIDEOS -
Male 8 Months Post-Op with 1 Session / 2535 Grafts to hairline & temporal recessions.
Watch our video gallery of client presentations...
see more!
Watch our video gallery of client presentations...
see more!
MALE | Norwood 4A - MALE PHOTOS -
Male 1 Year Post-Op with 1 Session / 3500 Grafts to frontal temporal recessions.
Preview our gallery of Before & After photos... see more!
Preview our gallery of Before & After photos... see more!
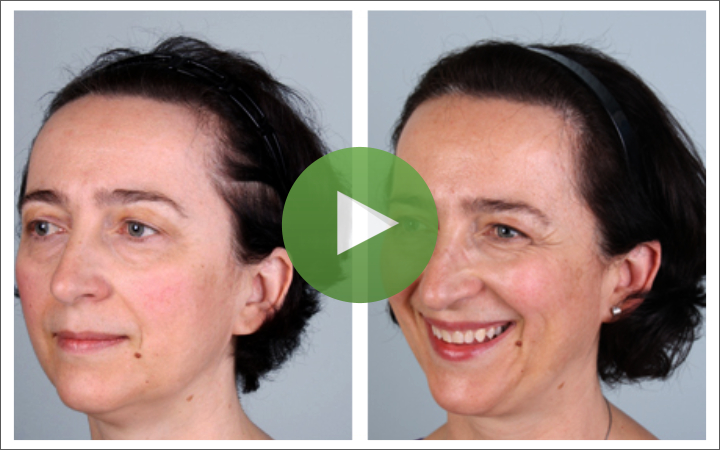
FEMALE | Ludwig II - FEMALE VIDEOS -
Female 1844 Grafts 1 Year Post-Op with 1 Session / 1844 Grafts to hairline & temporal recessions.
Preview our gallery of other Before & After female photos... see more!
Preview our gallery of other Before & After female photos... see more!
IN THE NEWS | TV - TV NEWS -
Dr. Cam Simmons was interviewed by Pauline Chan of CTV News about hair transplantats & techniques.
Watch other TV News... see more!
Watch other TV News... see more!
IN THE NEWS | RADIO - NEWS RADIO -
Listen to 640AM TalkRadio host Arlene Bynon and Dr. Cam Simmons discuss hair transplantation.
Listen to other radio interviews...
see more!
Listen to other radio interviews...
see more!